There has been a lot of controversy over the last decade or two about root canals. The disagreement is usually between dentists and root canal specialists (endodontists) on one side and alternative practitioners, like naturopaths, Integrative MD’s and chiropractors on the other. Dentists and endodontists almost always recommend saving the tooth. Alternative doctors usually land on the side of extraction.
Sometimes, the patient gets caught in the middle of this disagreement in philosophy and treatment approach. What is a patient to do? Read on and I think you will be pleasantly surprised and excited to find a new solution to the inherent problem with traditional root canal therapy.
The Problem
 According to an article published by the American Association of Endodontists (AAE) in 2011, current root canal solutions and techniques fail to completely remove all irritants and bacteria from the tooth during root canal therapy.
According to an article published by the American Association of Endodontists (AAE) in 2011, current root canal solutions and techniques fail to completely remove all irritants and bacteria from the tooth during root canal therapy.
The article discusses the complex nature of most root canal systems and why it is so difficult to remove bacteria completely from the canal system once it becomes infected. If bacteria is left behind after root canal therapy is complete, this sets up a problem for the future health of the tooth. According to the article:
Bacteria are the major cause of pulpal and periapical diseases. Complexity of the root canal system, invasion of the dentinal tubules by microorganisms, formation of smear layer during instrumentation and presence of dentin as a tissue are the major obstacles for complete elimination of bacteria during cleaning and shaping of root canal systems. The search for an ideal material and/or technique to completely clean infected root canals continues. (1)
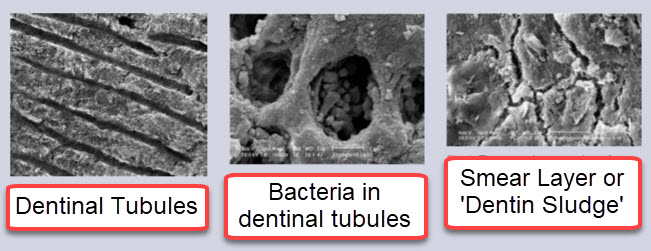 The article also presents three electron microscope images showing the problem in root canal therapy:
The article also presents three electron microscope images showing the problem in root canal therapy:
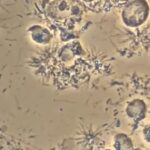
Image 1 shows the dentinal tubules that are in the root of every tooth, extending from the pulp to the outside of the tooth. It has been estimated that if these tubules are laid side by side they would extend between 1-3 miles in length, depending on the tooth.
Image 2 confirms what other investigators have reported: the presence of bacteria in the dentinal tubules of infected teeth. Bacteria have been found to populate up to half the distance of the tubule between the inside root canal and the outside of the tooth.
Image 3 shows that during root canal therapy a smear layer is created that covers the instrumented root canal walls of the tooth. This smear layer contains inorganic and organic substances as well as microorganisms (bacteria) and necrotic/toxic debris. (1)
Why you should care
According to the article above, root canal infections are dominated by E. faecalis, an anaerobic (oxygen-hating) bacteria that is resistant to intracanal medications, able to form biofilms and able to invade dentinal tubules. The article also states that, because the presence of bacteria negatively influences the outcome of root canal treatment, every effort should be made to eradicate infections during treatment. (1)
The second reason you should care is that there is research connecting E. faecalis with the incidence of heart disease. In a paper published in 2014 by the AAE in their professional publication (The Journal of Endodontics) the results showed that ‘patients with chronic apical periodontitis had a 2.79 times higher risk of developing coronary heart disease.’ (2) ‘Apical periodontitis’ means root canal infection, so the study concluded that people with chronic root canal infections have a 2.79 times greater chance of having heart disease than those that don’t.
To put this in perspective as a health concern, heart disease is the leading cause of death in America for both men and women. Over 600,000 men and women die from heart disease every year in the U.S., accounting for nearly 1 in 4 deaths. These are staggering statistics.
The Solution
According to Dr. Clifford Ruddle, one of the premier educators and trainers in root canal therapy in this country:
In the 40+ years that I have practiced and taught clinical endodontics, I have observed an awakening with the advent of the dental operating microscope, ultrasonically-driven instrumentation, NiTi files, and MTA. Recently, the renaissance has continued with the emergence of CBCT, 3D disinfection methods and the promise of regenerative endodontics.
Today, Photon-Induced Photoacoustic Streaming (PIPS) represents a leading advancement in laser-activated irrigation and disinfection. Any dentist who is committed to exquisitely cleaning root canal systems will definitely appreciate PIPS. This technology will not only send photoacoustic shockwaves through both minimally and fully prepared canals, but will also propagate shockwaves through our profession by promoting predictably successful results. — Clifford J. Ruddle, DDS
What is PIPS
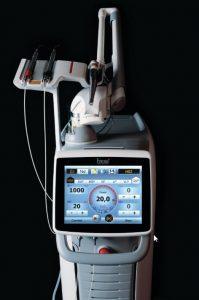 PIPS is short for Photon Induced Photoacoustic Streaming. It is part of the Advanced Laser Endodontic Therapy (ALET) that I offer at my practice in Encinitas, San Diego. PIPS when combined with ozone and SWEEPS, another and more powerful laser frequency, allows us to address the 3 problems listed above by the AAE:
PIPS is short for Photon Induced Photoacoustic Streaming. It is part of the Advanced Laser Endodontic Therapy (ALET) that I offer at my practice in Encinitas, San Diego. PIPS when combined with ozone and SWEEPS, another and more powerful laser frequency, allows us to address the 3 problems listed above by the AAE:
- Removes the bacteria and toxic, infected tissue from the canals of the roots
- Removes the smear layer from the canal walls that get caked on during treatment
- Cleans out bacteria and toxicity from the tubules
Pips harnesses the power of the Erbium laser to create photoacoustic shock waves, which thoroughly streams anti-bacterial and chelating solutions through the entire canal system. The canals and subcanals are cleansed and the dentinal tubules are left free and clear of the smear layer (tooth ‘sludge’).
How Effective is PIPS?
- When I do a root canal with PIPS and SWEEPS I can see the debris, sludge, and infection actively being flushed out of the tooth. In the protocol that I now follow, I rinse the tooth multiple times with PIPS and different cleaning and disinfecting solutions. By the time I’m done, the canals are clear and pristine. A well known M.D. I know says, ‘The solution to pollution is dilution.’ I find this to be true with PIPS and SWEEPS.
- A tooth I recently treated reminded me of the power of this technology. A patient came in with pain and swelling in his cheek from an infected tooth. So, I proceeded to treat the tooth with the PIPS and SWEEPS protocol. The next day I called him and when I asked him how his swelling was he replied, ‘It’s gone, doc.’ I asked, ‘It’s better, right?’ I did not really believe that it was fully gone, as it usually takes 3-5 days for a root canal infection to get better, even with antibiotics. Again he said, ‘Doc, I’m telling you, I’m good. The infection is totally gone.’ I was surprised, to say the least, and this was with no drugs or antibiotics.
 Research seems to support the above. Electron microscope analysis further confirms my clinical observations. This image shows an SEM image (left) and a microscope image (right) depicting bacteria in the microtubules of the tooth. The green lines are bacteria in the tubules made visible through staining.
Research seems to support the above. Electron microscope analysis further confirms my clinical observations. This image shows an SEM image (left) and a microscope image (right) depicting bacteria in the microtubules of the tooth. The green lines are bacteria in the tubules made visible through staining.
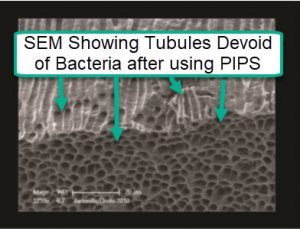 The SEM image to the left clearly shows that there are no bacteria present in the tubules after treating the same tooth with PIPS during Advanced Laser Endodontic Therapy. As you can clearly see the tubules are devoid of bacteria. This is nothing short of amazing, and I think is going to change how root canals are done in the future. Frankly, it’s one of the biggest advances I’ve seen in my 34 years as a dentist.
The SEM image to the left clearly shows that there are no bacteria present in the tubules after treating the same tooth with PIPS during Advanced Laser Endodontic Therapy. As you can clearly see the tubules are devoid of bacteria. This is nothing short of amazing, and I think is going to change how root canals are done in the future. Frankly, it’s one of the biggest advances I’ve seen in my 34 years as a dentist.
If you or someone you know would like your root canals evaluated, please call my office and speak with Victoria.
You can find out more about Advanced Laser Endodontic Therapy here: https://myholisticdentist.com/advanced-laser-endodontic-therapy-alet/
References for article:
- Collegues for Excellence. Root Canal Irrigants and Disinfectants, Winter 2011. Published for the Dental Professional Community by the American Association of Endodotists.
- Association between Chronic Apical Periodontitis and Coronary Artery Disease, Journal of Endodontics, Volume 40, Issue 2, February 2014, Pages 164-167, Tatiana Hassin RodriguesCostaMSc, et al.
- Efficacy of photon induced photoacoustic streaming (PIPS) on root canals infected with Enterococcus faecalis: A pilot study. Drs. David E. Jaramillo, et al explored whether the Er:YAG laser tip is an efficient tool in the elimination of Enterococcus faecalis from infected root canals

Carey O’Rielly DDS has been a practicing dentist for 35 years. He went to USC Dental School and Duke University for his undergraduate degree. He grew up in Laguna Beach and now lives in La Costa with his wife Victoria, who runs his office.
He began his career by owning and operating a network of six offices in the San Francisco Bay Area. Presently he owns a private holistic practice in North County San Diego’s Encinitas.
Dr. O started looking for solutions to his health challenges that resulted from the stress and environmental toxicity that built up over a ten year period running his dental network. He has dedicated himself to learning about oral systemic problems and how dentistry can affect your health. He has applied what he has learned over the last twenty years to ensure he, his staff and his patients are protected from the chemicals and toxic materials found in most dental offices. He has produced an environmentally friendly office that is also peaceful and calm.
He is an expert on dental materials having looked at hundreds of biocompatibility lab tests over the years. He has identified the most bio-friendly materials to use in his practice and which dental materials can be used to replace metal fillings and crowns, including BPA free and fluoride free ‘white’ fillings. He also uses metal-free Zirconia or ceramic implants and PRF (platelet-rich fibrin) grafting materials which come from the patient’s own blood.
Dr. O’Rielly teaches C.E. courses on the systemic effects of gum disease. He is an expert in using phase contrast microscopy for analyzing dental infections, where he shows patients what kind of microbes, i.e. bacteria, amoeba, and yeasts like candida are populating the mouth and affecting the body as a whole.
He has an educational blog and is writing a book on dental health called ‘Hidden Dental Infections: Healing Root Canals and Infected Teeth with the Erbium Laser’ where he discusses dental nutrition, toxic dental materials and the effects of old root canals on inflammation and overall health.